Sunlight provides many positive health benefits such as improving sleep, mood and mental health. It is also well known that sunlight helps keep our vitamin D levels optimal. But, how does sunlight specifically improve these factors, and what does “adequate” sunlight mean? Most individuals are not getting close to enough exposure to direct and indirectContinue Reading»

"Health Tips From Personal Trainer and Nutrition Specialist Jenni Berman..."
Use the Form Below to Get Them All Sent to You for FREE
Articles:
5 WAYS Physical Therapy Can Help After Meniscus Surgery You Need To Hear
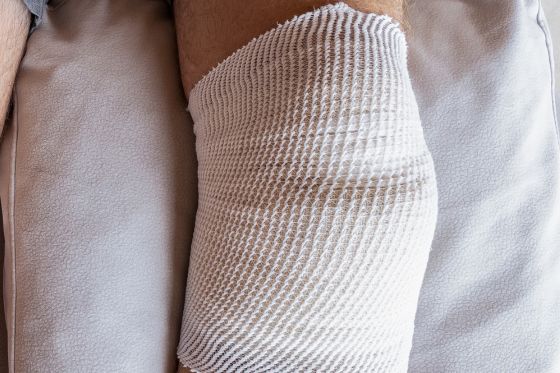
For many recovering from meniscus surgery, the journey back to full mobility is paved with uncertainty and discomfort. You may have expected to bounce back quickly, only to find yourself grappling with limitations that setback your recovery. If your post-surgery path has been rockier than anticipated, you’re not alone. Physical therapy (PT), often underprescribed post-surgery,Continue Reading»
Mastering Stress: A Comprehensive Guide to Lowering Cortisol Naturally Through Nutrition, Supplements, and Lifestyle Strategies
Stress. Like Taylor Swift at a football game, it gets talked about A LOT. But why? Let’s first understand what stress is at its core. What is Stress? Stress is cortisol. Cortisol is a steroid hormone that is produced in the adrenal glands (located above our kidneys). It can be healthy in the short termContinue Reading»
Taking Care of Your Mental Health
September is National Suicide Awareness Month, but every month should have focus on mental health. Mental Health is more prevalent than one thinks. According to recent studies: ● 1 in 5 adults in the United States live with mental illness ● In 2020, nearly 52.9 million adults were living with Mental Illness ● In 2022,Continue Reading»
Learn How to Use Your Body More Efficiently to Improve Golf Performance and Avoid Aches and Pains

Jake Berman here, and I’m reaching out to all of you who feel that your golf performance might not be quite up to par – pun intended. Is it a lack of distance on your drive? Or maybe it’s those nagging aches and pains that seem to follow every round, robbing you of the joyContinue Reading»
5 Keys to Success
Howdy – we are back for your next blog update! By the way – do you love these blogs? Are they helpful? If so, can you share them to a family member or friend who you think could benefit from reading? Would you be able to review our Google Page to let us know youContinue Reading»
How to Relieve Knee Pain at Night – 3 Tips for Better Sleep in the New Year

As we stand on the brink of a new year, I am struck by a thought that might resonate with many of you: I do not want to start 2024 with the same knee pain at night that plagued me in the past year. The idea of another year hampered by pain is disheartening.Continue Reading»
How to Improve Mobility and Health in Later Life! – 3 Expert Top Tips

The impact of becoming less mobile in our lives goes far beyond the physical limitations. Just think about the upcoming holidays – a time for joy, togetherness, and making cherished memories. Traveling to see loved ones, enjoying nature walks, and let us not forget, the simple act of putting on your favorite shoes to attendContinue Reading»
How To Treat Burning Knee Pain – 3 Expert Tips

The holidays are meant to be a time of joy, of family gatherings, of laughter and love. Yet, here I am, your friendly physical therapist, with a concern that is all too common: burning knee pain. It is that nagging, persistent discomfort that threatens to overshadow the holiday spirit, making you apprehensive about theContinue Reading»
Can Nutrition be Used as a Therapy in Crohn’s Disease?
The short answer to the title question is: Yes! But, Crohn’s Disease is a condition that can vary in severity and the same treatment plans do not apply for everyone with Crohn’s Disease. Each client needs a care plan tailored to their disease, symptoms and lifestyle. Crohn’s Disease is an autoimmune condition and isContinue Reading»
